|
The metaverse has the potential to radically transform the digital and global economy, shaping the world responsibly. With the metaverse in its early stages, organisations and people have the opportunity to shape the metaverse responsibly, revealed Mckinsey and Company, in its latest report. As per the report, the metaverse is an immersive, shared, and secure 3-D digital space where users’ avatar—a digital representation of oneself — can shop, play, learn, work out, attend virtual business meetings, trade digital currencies, and conduct other activities. Moving beyond its origin in gaming, the metaverse has already captured the interest of sectors such as fashion, art, and music. It is projected to reach $5 trillion in terms of value by 2030. “I believe absolutely that the advent of graphics-based computing and 3-D environments is going to change many of the technologies, standards, conventions, and monetisation models. It’s going to have profound generational change. And, most importantly, it’s going to reach many of the categories we’ve long hoped would be altered by mobile and the internet and yet haven’t been, ” said Matthew Ball, a venture capitalist, essayist, and observer of the digital world, wrote in the report. Ball further stated that the metaverse is a transformative event for the global and within that digital economy in many cases and further hoped that the metaverse and VR (virtual reality) and AR (augmented reality) will finally start to show actual, tangible, measurable productivity improvements in education and healthcare. For example, Johns Hopkins University recently performed its first pair of surgeries on live patients using augmented reality displays. The head of the neurosurgery and spinal department had described the experience as its like using GPS for the first time. “It’s not that it teaches you how to drive; it doesn’t drive the car for you, but you find that your ability to execute this task is much better than ever. Why does that matter as a use case? Well, not only is healthcare a costly industry, but like GPS and AR in surgery, it just needs to have a marginal impact on something of critical importance. It doesn’t need to perform the surgery; all we need is a meaningful increase to success rate,” Ball said. Augmented Realityfor Orthopedic Surgery The technology used by the physicians for the augmented reality surgeries consisted of a headset with a see-through eye display that projects images of the patient's internal anatomy such as bones and other tissue based on CT scans — essentially giving the surgeons X-ray vision PREVIOUS ARTICLES
0 Comments
Pfizer’s COVID-19 vaccine leads to lower levels of semen, according to a new study. Researchers analyzed 220 samples of semen from three sperm banks in Israel, drawn from men who received two doses of the vaccine. The semen collection was scheduled seven days after receipt of the second dose. The researchers, led by Dr. Itai Gat with the Sperm Bank and Andrology Unit at the Shamir Medical Center and Tel Aviv University’s Sackler Medical School, found that there was a decrease in sperm concentration between 75 and 120 days post-vaccination. The decrease led to a reduction in the motile count, or the number of sperm. Followup testing completed over 150 days after vaccination revealed “overall recovery,” with semen volume and sperm motility bouncing back, the researchers said. However, the levels outlined in the study were still lower than before vaccination. The peer-reviewed study was published online (pdf) ahead of being printed by Andrology. Pfizer did not respond to a request for comment. Gat told that a major strength of the study was the relatively long-term followup. “Overall we demonstrate long term safety of the vaccination regarding semen analysis among sperm donors. The temporary decline we found is similar to already known side effects of short febrile illness (ex. flu), followed by later recovery,” he said in an email. “It seems that the immune response after vaccination is similar as in cases of common infections which results with short term impairment of sperm production.” Previous research has indicated that getting sick with COVID-19 causes a change in the composition of semen, and that some illnesses can lead to sperm production being impaired. Men should only be concerned by the new research as much as they worry about similar issues arising after other infections, Gat said. “Obviously, most men are not aware of the short decline in their sperm counts after viral infection,” he said. Other studies conducted during the pandemic have found that sperm concentration and semen motility were not affected by COVID-19 vaccines, although Pfizer’s clinical trial included detection of anti-sperm antibodies. According to the U.S. Centers for Disease Control and Prevention, there is no evidence that vaccines affect fertility in women or men, despite the shots altering menstrual cycles in women. However, researchers acknowledge that the long-term impacts of the shots remain unknown, and won’t be known until longer-term studies are conducted. Gat wants to conduct further research on men who were vaccinated but described his team as lucky to have a large group of donors who were vaccinated during a short period of time. “When it comes to next doses, I expect timing diversity between donors, which will make further studies much more complicated,” he said. " In conclusion, in this longitudinal multicenter study, we found a selective temporary decline of sperm concentration and total motile count 3 months post-vaccination followed by recovery among SD. " credits to: By Zachary Stieber June 21, 2022 Updated: June 22, 2022 Epch Times Previous Articles
Using this diagnostic, doctors could avoid prescribing antibiotics in cases where they won’t be effective. Many different types of bacteria and viruses can cause pneumonia, but there is no easy way to determine which microbe is causing a particular patient’s illness. This uncertainty makes it harder for doctors to choose effective treatments because the antibiotics commonly used to treat bacterial pneumonia won’t help patients with viral pneumonia. In addition, limiting the use of antibiotics is an important step toward curbing antibiotic resistance. MIT researchers have now designed a sensor that can distinguish between viral and bacterial pneumonia infections, which they hope will help doctors to choose the appropriate treatment. “The challenge is that there are a lot of different pathogens that can lead to different kinds of pneumonia, and even with the most extensive and advanced testing, the specific pathogen causing someone’s disease can’t be identified in about half of patients. And if you treat a viral pneumonia with antibiotics, then you could be contributing to antibiotic resistance, which is a big problem, and the patient won’t get better,” says Sangeeta Bhatia, the John and Dorothy Wilson Professor of Health Sciences and Technology and of Electrical Engineering and Computer Science at MIT and a member of MIT’s Koch Institute for Integrative Cancer Research and Institute for Medical Engineering and Science. In a study of mice, the researchers showed that their sensors could accurately distinguish bacterial and viral pneumonia within two hours, using a simple urine test to read the results. Bhatia is the senior author of the study, which appears this week in the Proceedings of the National Academy of Sciences. Melodi Anahtar ’16, PhD ’22 is the lead author of the paper. Signatures of infection One reason why it has been difficult to distinguish between viral and bacterial pneumonia is that there are so many microbes that can cause pneumonia, including the bacteria Streptococcus pneumoniae and Haemophilus influenzae, and viruses such as influenza and respiratory syncytial virus (RSV). In designing their sensor, the research team decided to focus on measuring the host’s response to infection, rather than trying to detect the pathogen itself. Viral and bacterial infections provoke distinctive types of immune responses, which include the activation of enzymes called proteases, which break down proteins. The MIT team found that the pattern of activity of those enzymes can serve as a signature of bacterial or viral infection. The human genome encodes more than 500 proteases, and many of these are used by cells that respond to infection, including T cells, neutrophils, and natural killer (NK) cells. A team led by Purvesh Khatri, an associate professor of medicine and biomedical data science at Stanford University and one of the authors of the paper, collected 33 publicly available datasets of genes that are expressed during respiratory infections. By analyzing those data, Khatri was able to identify 39 proteases that appear to respond differently to different types of infection. Bhatia and her students then used those data to create 20 different sensors that can interact with those proteases. The sensors consist of nanoparticles coated with peptides that can be cleaved by particular proteases. Each peptide is labeled with a reporter molecule that is freed when the peptides are cleaved by proteases that are upregulated in infection. Those reporters are eventually excreted in the urine. The urine can then be analyzed with mass spectrometry to determine which proteases are most active in the lungs. The researchers tested their sensors in five different mouse models of pneumonia, caused by infections of Streptococcus pneumoniae, Klebsiella pneumoniae, Haemophilus influenzae, influenza virus, and pneumonia virus of mice. After reading out the results from the urine tests, the researchers used machine learning to analyze the data. Using this approach, they were able to train algorithms that could differentiate between pneumonia versus healthy controls, and also distinguish whether an infection was viral or bacterial, based on those 20 sensors. The researchers also found that their sensors could distinguish between the five pathogens they tested, but with lower accuracy than the test to distinguish between viruses and bacteria. One possibility the researchers may pursue is developing algorithms that can not only distinguish bacterial from viral infections, but also identify the class of microbes causing a bacterial infection, which could help doctors choose the best antibiotic to combat that type of bacteria. The urine-based readout is also amenable to future detection with a paper strip, similar to a pregnancy test, which would allow for point-of-care diagnosis. To this end, the researchers identified a subset of five sensors that could put at-home testing closer within reach. However, more work is needed to determine if the reduced panel would work similarly well in humans, who have more genetic and clinical variability than mice. Patterns of response
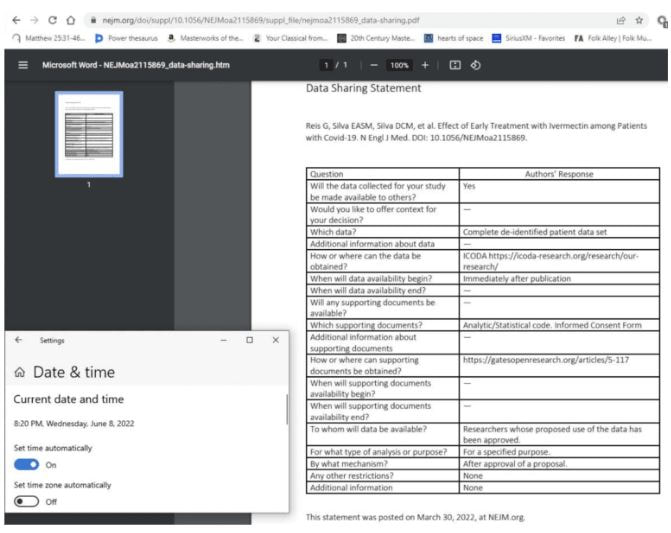
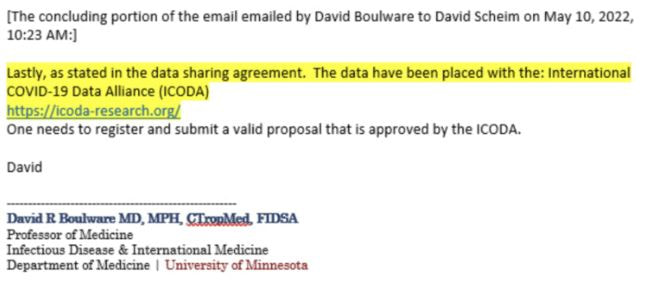
In their study, the researchers also identified some patterns of host response to different types of infection. In mice with bacterial infections, proteases secreted by neutrophils were more prominently seen, which was expected because neutrophils tend to respond more to bacterial infections than viral infections. Viral infections, on the other hand, provoked protease activity from T cells and NK cells, which usually respond more to viral infections. One of the sensors that generated the strongest signal was linked to a protease called granzyme B, which triggers programmed cell death. The researchers found that this sensor was highly activated in the lungs of mice with viral infections, and that both NK and T cells were involved in the response. To deliver the sensors in mice, the researchers injected them directly into the trachea, but they are now developing versions for human use that could be administered using either a nebulizer or an inhaler similar to an asthma inhaler. They are also working on a way to detect the results using a breathalyzer instead of a urine test, which could give results even more quickly. The research was funded, in part, by the Bill and Melinda Gates Foundation, Janssen Research and Development, the Koch Institute Support (core) Grant from the National Cancer Institute, and the National Institute of Environmental Health Sciences. Original Article: Anne Trafton | MIT News Office PHOENIX, Ariz. — Headache disorders are among the most common health problems worldwide and one of the most underdiagnosed and undertreated, according to the World Health Organization (WHO). In this expert alert, neurologist Amaal Starling, M.D., a headache and migraine expert at Mayo Clinic in Phoenix, offers tips to prevent and manage headache disorders, including migraine and medication-induced rebound headache. There are more than a dozen different types of headache disorders. The most common disabling headache disorder is migraine. It affects more than 1 billion people around the globe, including 1 in 5 women, 1 in 11 children and 1 in 16 men, and according to WHO, is one of the world’s most disabling diseases, Dr. Starling says. Migraine disease can differ depending on a person’s stage in life, she says. “Infant colic is thought to be the infant variant of migraine. Abdominal migraine and cyclic vomiting syndrome are migraine variants that are common in children,” Dr. Starling says. “More classic migraine attacks occur throughout adulthood. In the older adult, the pain associated with migraine lessens; however the associated features such as light sensitivity, sound sensitivity, nausea, vomiting, or aura may be more prominent.” Despite advances in treatment and prevention options, migraine remains underdiagnosed and therefore undertreated, Dr. Starling says. If someone has head pain that makes it difficult to function, odds are that it is migraine; often people think they have sinus headache when it is really migraine. Migraine is a primary headache disorder, meaning it is caused by abnormal function in the brain. Unlike secondary headache disorders, it may not be a symptom of an underlying illness such as an infection or a tumor. Other common primary headache disorders include cluster headache, which occurs in bouts of attacks lasting from weeks to months and typically includes intense pain lasting up to three hours in or around one eye; and tension headache, which usually comes with mild to moderate pain and can be chronic. Some primary headache disorders are associated with certain activities, such as cough headache, sex headache and exercise headache. They also can be triggered by drinking alcohol, eating certain foods such as processed meats containing nitrates, lack of sleep, poor posture, stress and missed meals. “Migraine triggers are very individualized. A trigger for one patient may not be a trigger for the next patient,” Dr. Starling says. “In general, I recommend eating an anti-inflammatory Mediterranean-style diet with fruits, veggies, nuts, legumes; eating foods high in magnesium, eating whole foods, and avoiding processed foods and fasting,” she says. “More recently there has been some data that recommend consuming more omega-3 fatty acids by eating fatty fish such as salmon, sardines, and mackerel.” Overuse of pain medication, including taking nonprescription analgesics such as aspirin and acetaminophen or prescription medications such as opioids and some migraine medications more than twice a week, can trigger rebound headache, also known as medication overuse headache. “If someone is having migraine attacks four or more times a month, it is time to consider preventive treatment,” Dr. Starling says. “If someone has infrequent migraine attacks, occurring less than four times per month, a migraine-specific treatment as needed may be more effective than over-the-counter analgesic medications such as ibuprofen.” New treatments for migraine include the discovery of a new family of preventive medications that target one of the body’s systems believed to be a culprit, the calcitonin gene-related peptide system, and the development of medical devices to treat migraine, she says. If patients have head pain that is reducing their ability to function, rather than diagnosing themselves and self-medicating, it is best to see a health care provider for help managing symptoms, Dr. Starling says. “Over the past several years there has been an explosion of treatment options for migraine attacks and migraine prevention,” she adds. “We have many treatment options to improve the lives of those living with migraine.” Sharon Theimer Mayo Clinic Public Affairs, PREVIOUS ARTICLES: -World Council for Health Following the release of the TOGETHER Trial results to the press in August 2021, media headlines quoted that ivermectin had ’no effect whatsoever’ when used for Covid-19. This press release from TOGETHER Trial investigators influenced international health policy to withhold ivermectin for the prevention and treatment of Covid-19 despite compelling evidence from numerous independent experts, scientific papers, and real world data that mass administration of ivermectin would be effective and safe for Covid-19. The final report of the TOGETHER Trial, published in March 2022 in the New England Journal of Medicine, has major discrepancies in the data compared with what was published by the media more than six months earlier in addition to serious methodological inconsistencies that must be brought to light. Despite numerous requests by international scientists to address these issues, none has been forthcoming by TOGETHER Trial authors. Probable Scientific Misconduct UncoveredA breaking development has highlighted the probability of scientific misconduct associated with this trial, when the manager of the International COVID-19 Data Alliance (ICODA) confirmed that its website, to which the TOGETHER trial has been directing inquiries for deidentified patient data since the study’s publication on March 30, never actually hosted the study’s data. Dr. David Scheim, Dr. Edmund Fordham, and Professor Colleen Aldous have sent a letter (part of which is included below) to the TOGETHER Trial authors, the NEJM Editor-in-Chief, and others asking for the data to be made available immediately or to retract the paper. Call for ActionThis is not the first time that attempts have been made to manipulate data and scientific manuscripts to undermine the evidence that shows ivermectin is effective against Covid-19. The World Council for Health urges journalists, scientists, and civil society to focus due attention on TOGETHER Trial investigators so that they reveal what has been hidden. The World Council for Health supports the use of ivermectin for the prevention and treatment of acute Covid-19, Long Covid, and for Covid-19 vaccine injury under the supervision of trusted health practitioners. BREAKING: The TOGETHER trial data was never at its cited ICODA repository or otherwise availableDear coauthors of Reis et al., 2022,1 the Editor-in-Chief of the New England Journal of Medicine; and (cc’d) editors of other scientific journals, science reporters, bioethicists and other distinguished scientists: In a breaking development yesterday, we learned that the TOGETHER trial has misdirected inquiries to a web repository that never hosted its data, thereby denying the scientific community access to the underlying data for its ivermectin arm since that study’s publication on March 30. A manager of the ICODA data repository emailed us yesterday that its website, to which the TOGETHER trial has been directing inquiries for deidentified patient data since the study’s publication on March 30, never hosted the study’s data. This took two months to ascertain, in part because ICODA’s listed telephone number still gives the recorded message, “you have reached a number that is not currently set up to receive calls.” Given this flagrant breach of scientific ethics in thwarting access to data with a spurious link, the four outcome measures that scientists have repeatedly requested since April 11, comparative per protocol death and hospitalization rates, treatment vs. placebo, should be disclosed immediately. Note that these are the key outcomes of interest, since both the NIH and FDA found the study’s nonstandard primary outcome measure to be inadequate. It is especially troubling that study co-author Dr. David Boulware evaded our May 10 request for the study’s four key outcome numbers (email thread below) by misdirecting, once again, to this spurious link to ICODA, which never hosted the TOGETHER trial’s data. The degree of data irregularities and concealment of data here is of a scale unmatched since the Surgisphere scandal of June 2020, which resulted in retractions in the New England Journal of Medicine (NEJM, the publisher of this March 30 study) and in the Lancet.
As noted, the study coauthor cited above who replied twice in response to our May 10 letter could not furnish even the simplest accurate information about the study data, its repository location. It is therefore imperative that a study coauthor who can accurately report on this data immediately disclose to the scientific community the four numbers for comparative per protocol death and hospitalization rates as repeatedly requested since April 11. Expedited access to “complete deidentified patient data,” as the study promised beginning “immediately after publication,” on March 30, must also be provided. If these are not provided promptly, we request that the NEJM retract this study. Sincerely yours, David E. Scheim, PhD, US Public Health Service, Commissioned Corps, Inactive Reserve, Blacksburg, Virginia, USA Colleen Aldous, PhD, MASSAf (fellow, Academy of Science, South Africa), School of Clinical Medicine, College of Health Sciences, University of KwaZulu-Natal, Durban, South Africa Edmund J. Fordham, PhD (Cantab) FInstP, EbMCsquared CiC, Bath, England
Digital Medical Certificate, AltHash Health Blockchain
With the Pandemic much falsified medical certificate has been spreading. The blockchain-based database provides authenticity, immutability, and security of Data. Hence, it is but logical that medical certificates be stored in the blockchain. It also maintains Data Privacy. Last 2018-19 we introduced this project to the Philippines.
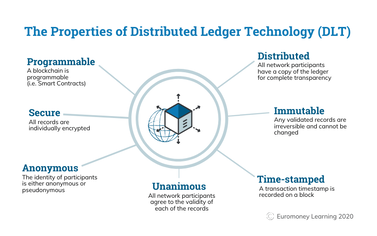
What is the main purpose of blockchain?
The goal of blockchain is to allow digital information to be recorded and distributed, but not edited. In this way, a blockchain is the foundation for immutable ledgers, or records of transactions that cannot be altered, deleted, or destroyed.
Blockchain is an emerging technology being applied for creating innovative solutions in various sectors, including healthcare. A Blockchain network is used in the healthcare system to preserve and exchange patient data through hospitals, diagnostic laboratories, pharmacy firms, and physicians.
Is there a healthcare blockchain?
At this time, the most common use cases of blockchain in healthcare leverage smart contracts capabilities for medical supply chain, health-credential and vaccination validation, provider credentialing, patient data security, and life sciences clinical study-related data.
The problem in Medical Certificate Issuance experienced in the Philippines One of the challenges in the issuance of medical certificates is the falsification of the document. Doctors most of the time receive inquiries and complaints from health insurance companies or the human resource departments on the certificates submitted by the sick employee. Often times the company doctor or nurse be it from HR/School? or insurance would have to confirm or call the issuing physician on the diagnosis, medication, or recommendation written in the medical document. This oftentimes causes doubt about the credibility of the Doctor. Worst case scenario is when a crime is committed by manufacturing fake medical certificates using an innocent doctor's name and his medical license. This recently happened in Quezon City. 
An article by CNN about the problem
""Police raid print shop producing fake medical certificates of COVID-19 results( Metro Manila (CNN Philippines, July 23) Police on Thursday raided a printing shop in Quezon City for allegedly producing fake medical certificates of COVID-19 results. The Quezon City Criminal Investigation and Detection Group (CIDG) organized an entrapment operation in the afternoon at Brgy. Pasong Putik after a social media post went viral exposing the scheme. Authorities arrested two employees and confiscated the printers, computers, and other hardware as evidence." Full Article. Read More....
IT IS A CRIME
Section 1. Article 174 of Section 5, Chapter 1, Title IV of Act No. 3815 FALSIFICATION OF MEDICAL CERTIFICATES IS A CRIME AND IS PUNISHABLE BY LAW Penalty: The penalties of [arresto mayor] PRISIONCORRECCIONAL in its maximum period to [prision correccional] PRISION MAYOR in its minimum period and a fine not to exceed [1,000] TWO HUNDRED THOUSAND PESOS (P200,OOO.OO) WITH SUBSIDIARY IMPRISONMENT This is where we come in, Digital Medical Certificate
A secure, private and confidential way of creating Medical Certificate by a Medical Doctor. It gives practicing physicians the assurance that their issued certificates, were not corrupted, falsified. Likewise for the Human resource department who receives the medical certificate that the document is true and authentic
Why is Blockchain based Medical Certificate Secure?
Key things: a. Data is cryptographically stored using SHA 256 or Secure Hash Algorthm "SHA-256 stands for Secure Hash Algorithm 256-bit and it's used for cryptographic security. Cryptographic hash algorithms produce irreversible and unique hashes. The larger the number of possible hashes, the smaller the chance that two values will create the same hash. It is developed by NSA" 
Hashing is the process of scrambling raw information to the extent that it cannot reproduce it back to its original form. It takes a piece of information and passes it through a function that performs mathematical operations on the plaintext. This function is called the hash function, and the output is called the hash value/digest.
b. the cryptographic data can be decrypted using a private and public key Ecnycryption,
" Only the owner of the private key can encrypt data so that the public key decrypts it; meanwhile, anyone can encrypt data with the public key, but only the owner of the private key can decrypt it. Therefore, anyone can send data securely to the private key owner."
c. The Encrypted Data is stored in a distributed ledger an independent, autonomous node of computers.
For a Criminal to corrupt the Data stored in the MEdical Certificate done by the private physician he has to:
a. decrypt the SHA 256 " As of 2021 technology, the chance of solving a hash with SHA256 algorithm, that is, converting it to the main input, is very very low possibility" b. access the private key of the issuing Doctor " Hackers can infiltrate wallets and steal bitcoins if they know a user's private key." c. hack all the autonomous, anonymous, distributed nodes (all over the globe) which participated in the blockchain network. not including the consensus mechanism of verification on each block. "A blockchain's decentralized nature means that its network is distributed across multiple computers known as nodes. This eliminates a single point of failure. In other words, there is no way to “cut the head off the snake” — because there isn't any head." WATCH DEMO VIDEO ON DAPP (DECENTRALIZED APPLICATION) DIGITAL MEDICAL CERTIFICATE
Blockchain used cases in healthcare to preserve the integrity of the document, and integrity of Physicians and save a lot of money for Companies and insurance paying for fake/falsified documents.
Only a licensed Medical Doctor can have access to and create the Certification. AltHash follows strict background checks to confirm Physicians' application to use the AltHash Health Blockchain

Dr. vincent Rey Vicente, MD is a practicing medical professional, a senior faculty of AltHash University. At present he is also the Business Developement Director of theInternationcouncil of Registered Blockchain Professionals (ICORBP). He introduced Digital Medical Certificate to private medical practices in Davao City, Philippines in addition to the Digital Birth Certificate.
The lining of your digestive tract — like every surface of your body — is covered in microorganisms, mostly bacteria. This microecosystem, called a microbiome, plays a large role in your health. Your mood and behavior also may be impacted by the microorganisms living in your microbiome.
You may be surprised to hear your gut houses up to 1,000 different species of bacteria. By nourishing different types of bacteria, you can keep your microbiome in balance. What you feed your microbiome matters. Most healthy adults can safely incorporate prebiotics and probiotics to their diet. A healthy microbiome promotes a healthy immune system and supports a weight management plan.
There are two ways to maintain a healthy gut:
In a large bowl, combine the oats and hot water. Let sit for 1 to 2 minutes until the oats are creamy and tender. Stir in oil and sugar; set aside to cool slightly. In a medium bowl, combine the flours, baking powder, baking soda, salt and ground cinnamon. Whisk to blend. Add the milk, yogurt and banana to the oats and stir until well-blended. Beat in the egg. Add the flour mixture to the oat mixture and stir until just moistened. Place a nonstick frying pan or griddle over medium heat. Once hot, spoon ¼ cup pancake batter into the pan. Cook for about 2 minutes, until the top surface of the pancake is covered with bubbles and the edges are lightly browned. Flip the pancake and cook for another 2 to 3 minutes. Repeat with remaining pancake batter.
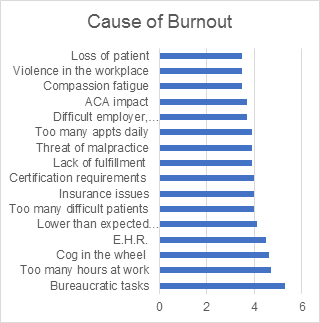
Nutrition information per two-pancake serving: 192 calories, 6 grams fat, 0 grams saturated fat, 0 grams trans fat, 4 grams monounsaturated fat, 302 milligrams sodium, 30 grams total carbohydrate, 2 grams dietary fiber, 6 grams protein You may also be interested in other articles:When physicians lament they feel burned out at work, what exactly do they mean?  Here's how one doctor describes conditions that lead to burnout: "I barely spend enough time with most patients, just running from one to the next; and then after work, I spend hours documenting, charting, dealing with reports. I feel like an overpaid clerk." Physicians experiencing work burnout don't always find relief at home. "Home is just as busy and chaotic as work. I can never relax," another physician says. The Medscape Physician Burnout & Depression Report 2022: Stress, Anxiety and Anger report sparked impassioned responses from physicians on several fronts. In that report, 47% of physicians who responded said they were experiencing burnout, up from 42% in our survey from 2021. Few Doubt the Burnout/Depression ProblemWhile opinions differ about the chief culprits, commenters lamented rather than questioned the extent of burnout and depression among physicians. "What is striking to me is, 24% of our colleagues are suffering from clinical depression," one doctor worried. "This is a serious matter. Individuals need to address a work-life balance. Find ways to seek help, and [develop] a coping mechanism."
"I am sympathetic, but medical schools should do a better job in choosing and teaching students that being a doctor requires having a vocation for it. That's not the same as being a do-gooder," one physician argued. "It's having a passion for medicine and practicing it." The Right Employer and Community Help DoctorsHow possible is it to put together the right combination of employer and vibrant community that avoids burnout? That question generated a lively back-and-forth. "Get your degree, do your residency, then say goodbye to corporate medicine and do direct primary care," one doctor advised. "You will pay off your loans and have fun doing it!" Another physician shot back, "Good luck launching an independent practice in a community with amenities that let you lead a full and enjoyable life away from work." Certainly research shows a healthy work-life balance and a rewarding personal life positively affect burnout and depression among physicians. Some believe relaxation is more attainable in self-employment vs corporate employment, but that assumption has not always proved true. The right choice for a doctor's mental health is sometimes elusive and is affected by many factors. Credits:
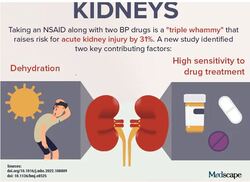
Images: E+/Getty Images Medscape Medical News © 2022 Cite this: Jon McKenna. Physicians React: Burnout Rates Are Alarming, so Who Should Drive Change? - Medscape - Jun 06, 2022. A new study investigating a dangerous "triple whammy" in patients taking blood pressure (BP) medications, research into complications from cancer regimens, and recent findings about treatment and prevention concerns resulted in kidneys becoming this week's top trending clinical topic. The combination of three drugs — a diuretic; a renin-angiotensin system inhibitor, such as an angiotensin-converting enzyme (ACE) inhibitor or angiotensin receptor blocker; and a nonsteroidal anti-inflammatory drug (NSAID) — increases the risk for kidney injury. New research has identified the mechanism responsible (see Infographic). Not all patients who take the "triple whammy" combination develop kidney problems. To better understand the mechanism responsible for injury, researchers used computational models to gauge interactions. Their simulations suggested that low water intake, the myogenic response, and drug sensitivity may predispose certain patients to develop triple whammy–induced acute kidney injury. Without these additional risk factors, the risk was not elevated when an ACE inhibitor and NSAID were combined. In contrast, when an ACE inhibitor, diuretic, and NSAID are combined, critical BP and estimated glomerular filtration rate (eGFR) regulatory mechanisms are simultaneously interrupted. The "triple whammy" isn't the only drug combination that creates kidney concerns. A preprint study that has not yet been peer-reviewed examined which colorectal cancer regimens are most likely to result in acute kidney injury. The most likely culprit was FOLFIRI + bevacizumab. Prognostic factors included older age, low body mass index, and proteinuria at baseline. Across the four included regimens, patients' median eGFR fell from 90.9 mL/min/1.73 m2 at baseline to 80.1 mL/min/1.73 m2 at 12 months. Median 12-month eGFR among the 97 patients receiving FOLFIRI + bevacizumab fell the most, to 74.9 mL/min/1.73 m2. Incidence of acute kidney disease was lowest among patients treated with FOLFOX + cetuximab (2.1%) and highest among those who received FOLFIRI + bevacizumab (19.2%). In more encouraging kidney news, a recent study found that risks are low for donors. According to what is believed to be the largest study to date to examine the risks associated with living kidney donation via hand-assisted laparoscopic nephrectomy, the overall rate of complications was lower than that reported in some larger databases. Among 3002 living kidney donor nephrectomies, the overall complication rate was 12.4% (n = 371). Most were an infection or hernia related to the incision. The incidence of major complications was 2.5% (n = 74). Of these, 15 were intraoperative, 12 were postoperative to discharge, and 47 occurred after discharge to day 120 (all were reoperations, of which 46 were related to incisional issues). Not all kidney treatment-related news is as positive. A qualitative study recently found that Black veterans who have chronic kidney disease (CKD) report emotional and physical stress caused by racism in the medical setting. Researchers interviewed 36 Black veterans with CKD who were receiving care at the Corporal Michael J. Crescenz Veterans Affairs Medical Center. The mean age of participants was 66 years, and men comprised 97% of the study group. The qualitative data showed that Black veterans experienced physiologic symptoms (eg, headaches) and psychological symptoms of hurt and anger. They also felt a need to be hypervigilant during medical visits, which may be indicative of posttraumatic stress disorder. Outside of medical facilities, certain interventions may be beneficial in slowing kidney function decline. According to an analysis of randomized clinical trials, a structured moderate-intensity physical activity and strength/flexibility program in older adults (mean age, about 79 years) benefited kidneys. The program resulted in a statistically significantly lower decline in eGFR rate per cystatin C (eGFRCysC) compared with health education alone (mean difference, 0.96 mL/min/1.73 m2) and lower odds of rapid eGFRCysC decline (odds ratio, 0.79). Patients in the intervention arm underwent a structured, 2-year, partially supervised, moderate-intensity physical activity and exercise (strength and flexibility). Those in the health-education control arm attended weekly workshops. Cite this: Ryan Syrek. Trending Clinical Topic: Kidneys - Medscape - May 27, 2022.
By Susan Buckles Mayo Clinic Vulnerability to heart disease can be projected before symptoms occur, Mayo Clinic discovered in preclinical research. This proof-of-concept study revealed that heart muscle changes indicate who is vulnerable to disease later in life. These changes can be detected from blood samples through comprehensive protein and metabolite profiling. This exploratory mapping, conducted in the Marriott Family Comprehensive Cardiac Regenerative Program within Mayo Clinic's Center for Regenerative Medicine, is published in Scientific Reports. "The team implemented state-of-the-art technologies to predict who is vulnerable and who is protected from heart disease," says Andre Terzic, M.D., Ph.D., a Mayo Clinic cardiologist and the senior author. "In this era of post-genomic medicine, the acquired foundational knowledge provides guidance for development of curative solutions targeted to correct the disease-causing maladaptation." Dr. Terzic is the Marriott Family Director, Comprehensive Cardiac Regenerative Medicine, for the Center for Regenerative Medicine and the Marriott Family Professor of Cardiovascular Research. Heart disease is a leading killer in the U.S., responsible for 1 of every 4 deaths, according to the Centers for Disease Control and Prevention. Predicting and intervening early in heart disease are health care priorities aimed at improving survival and quality of life while reducing health care costs. To address unmet needs of patients with chronic conditions such as heart disease, Mayo Clinic has invested in regenerative medicine and individualized medicine, transformative emerging fields in modern health care. Regenerative medicine seeks to restore the form and function of a failing or diseased organ, with individualized medicine tailoring care to a person's makeup. Mayo Clinic's Center for Regenerative Medicine is prioritizing clinical-grade biotherapeutics, targeting diseases with no cure. The research D. Kent Arrell, Ph.D. D. Kent Arrell, Ph.D. The research team mapped the molecular composition of hearts and discovered that in young adults, despite absence of any overt cardiac malfunction, deficiency in KATP channels -- innate safeguards of cardiac cell well-being under stress load — triggered heart tissue alterations that predict increased disease susceptibility. "We found that KATP channel deficit reorganizes the molecular identity of the heart. Notably, salient changes were also evident in blood, suggesting that heart vulnerability may be detected with a blood test, avoiding the need for invasive tissue biopsy," says D. Kent Arrell, Ph.D., first author. "Blood biomarkers could inform targeted biotherapeutic interventions for individuals deficient in natural cardiac protective capability." The team took a multiomics, high-tech systems approach to map the multiplicity of molecular changes. Going beyond the genome, thousands of distinct proteins and metabolites were deciphered, drawing a molecular atlas of cardioprotective deficiency.  Satsuki Yamada, M.D., Ph.D. Satsuki Yamada, M.D., Ph.D. "This proactive approach prior to disease onset offers an opportunity to maximize the success of future biotherapies aimed at addressing life-threatening conditions by correcting pinpointed deficits early in life that can be tailored for each individual," says Satsuki Yamada, M.D., Ph.D., a cardiologist and member of the study team. Future clinical studies will be needed to translate these findings and ultimately advance diagnostics capable of predicting the risk of heart disease. |
AUTHOR
An approach to healing that considers the whole person -- body, mind, spirit, and emotions -- in the quest for optimal health and wellness. Most of the time I share articles from different journals with atributions and sometimes I write articles. LISTEN TO SOOTHING LOFI FOCUS MUSIC. Play BELOW
Boost your immune system with intraArchives
April 2023
|




























 RSS Feed
RSS Feed




